NF1-related plexiform neurofibromas (PN) are benign tumors that can have a significant impact on children. Knowing more about the disease can allow you to have more informed conversations with your child’s doctor. As a parent or caregiver, being knowledgeable about your child’s condition is one of the best ways you can help them through their journey.
This website is designed to help you better understand NF1 PN. We encourage you to share what you learn with other parents of children with NF1 PN.
NF1 PN:
What You Need To Know
What is neurofibromatosis type 1 (NF1)?
NF1 is a progressive, genetic condition that is caused by a mutation or flaw in a particular gene. Symptoms and onset of major clinical manifestations of NF1 occur mostly from birth to 18 years. It occurs in approximately 1 out of every 3000 individuals.
What are plexiform neurofibromas (PN) that are associated with NF1?
Plexiform neurofibromas, sometimes referred to as plexiform tumors, are benign (noncancerous) tumors that can grow along nerves anywhere in the body.
Up to 50% of children with NF1 have plexiform neurofibromas (PN) identified based on full-body MRI scan.
Why should caregivers look out for plexiform neurofibromas (PN)?
PN can grow along any nerve, so they can negatively affect any parts of the body. Some PN are also progressive, meaning that they continue to grow.
Some children do not experience progression. They may have manifestations that seem to stay the same and do not change significantly over time.
In a study following children with NF1, it was found that 3 out of 4 children experienced PN growth ≥20%.*
*Based on a National Cancer Institute NF1 Natural History study of 93 patients with a median observation period of 6.8 years (range: 1 to 17.7 years).
PN can quickly grow to larger sizes and may start to cause symptoms, including:
-
Visible cosmetic changes
-
Pain
-
Numbness
-
Weakness
-
Mobility issues
Early identification is important
PN aren’t always easy to notice in children with NF1. Sometimes they are located deep inside the body, so they can’t be seen or felt under the skin. In some cases, the first sign may be skin discoloration or a bump under the skin. Identifying PN early means that your child’s doctor can start to create an appropriate treatment plan.
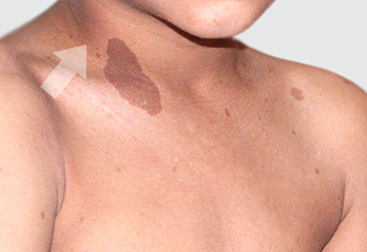
Plexiform neurofibromas on the right side of neck.
It’s important to look out for
physical
signs of PN
that may be
impacting your child
MRI=magnetic resonance imaging.
TREATMENT FOR NF1 PN
Which doctors or specialists usually treat NF1?
NF1 is usually managed by a team of doctors and healthcare specialists, including but not limited to:
-
Dermatologists
-
Oncologists
-
Neurologists
-
Surgeons
-
Orthopedists
Other providers who specialize in treating symptoms related to NF1 PN may also be part of the treatment process. Having a team of doctors can help ensure that all of your child’s needs are being addressed.
Can surgery help treat PN?
PN form differently in every child, and some can be removed by surgery to improve appearance or function. Enlarging plexiform neurofibromas may be managed surgically. If surgery can be performed, repeat surgeries may be needed because PN tend to regrow, especially if they cannot be completely removed.
Plexiform neurofibromas can be large or small and can appear in various places around the body. Some PN are considered inoperable, meaning they cannot be totally removed by surgery. For example, they may:
-
Become intertwined with important nerves
-
Grow near vital organs
-
Develop in areas of the body that are especially hard to operate on (such as the head, neck, or spine)
-
Become full of blood vessels, which can lead to bleeding during surgery
Your healthcare team may decide whether surgery is recommended based on a careful study of your child’s particular case and treatment plan. Early identification of PN can help your child’s healthcare provider determine the best plan of action.
Are there any other ways to treat plexiform neurofibromas?
Your child’s doctor may prescribe therapy or medicines to help with symptoms of NF1, including:
-
Pain
-
Lack of mobility
-
Reduced range of motion
LIVING WITH NF1 PN
What are some of the physical challenges associated with NF1 PN?
PN can vary widely in their shape, size, and location. They can cause a number of potential complications throughout the body, including:
Pain
PN can press on nerves or organs,
causing pain, weakness, or numbness
Restricted motion
Physical mobility, range of motion, and
strength can be limited by PN
Vision impairment
PN can sometimes develop in or
near the eye area, which can cause vision disturbances
Breathing problems
If PN grow in the chest area, they can
begin to cause breathing problems
Visible cosmetic changes
PN can grow in different sizes and
in various locations around the body,
including
the face or neck, where they
can be more easily noticed
Constipation and incontinence
PN that are located on or near
the spine may result in bladder and bowel problems
How can I help my loved one with NF1 PN?
Living with NF1 can be difficult for both patients and caregivers, especially when plexiform neurofibromas (PN) are present. Here are some ways you can help your child better cope with the challenges:
Create daily routines
NF1 can cause a lot of uncertainty, so creating schedules can help children feel more secure and give them a sense of control.
Make treatment easier
Getting children to take medicine every day can be hard, but helping them understand why it’s important and encouraging them with positive reinforcement can help them feel empowered.
Come together as a family
A diagnosis of NF1 PN can affect the entire family. Building a supportive home environment can benefit everyone, including siblings who may feel that they’re not getting as much attention.
Ease the transition into teenage years
As children grow into teenagers, they can become more active participants in their own care. Allowing them to take more control over their treatment decisions and medications can encourage greater responsibility.
Take care of yourself
As a parent or caregiver, you do everything you can to help your child with NF1 PN. But it’s also important to take some time for yourself and to reach out for support when needed.
Connect with the NF1 community
There are several patient advocacy groups that can provide information and support to families who are dealing with NF1.

The mission of the Children’s Tumor Foundation is to drive research, expand knowledge, and advance care of the NF community. Visit >

Visit the Neurofibromatosis Network website to discover news about treatment and their work toward a neurofibromatosis cure. They provide outreach through education and awareness, while offering hope and support to those affected by NF. Visit >

The Littlest Tumor Foundation is focused on increasing the understanding of neurofibromatosis (NF), empowering affected families, and advancing research of preventative therapies. Visit >
The advocacy resources listed above are independent, nonprofit patient service organizations. Their listing on this website does not imply endorsement. All logos and trademarks are the property of their respective owners.
A diagnosis of NF1 PN can be
life-changing for patients and their
families.
But learning more about the
condition and maintaining an open
dialogue with your
child’s healthcare
team can make a big difference in
your child’s journey.
And there’s reason to be hopeful—NF1
research is ongoing, with the
goal of developing treatments for
children affected by this rare disease.
NF1 with Plexiform Neurofibromas (PNs): What You Need To Know
What is neurofibromatosis type 1 (NF1)?
NF1 is a rare, progressive condition caused by a mutation or flaw in a particular gene. NF1 is usually diagnosed in early childhood. It appears in an estimated 1 out of every 3000 infants.
What are plexiform neurofibromas (PNs) associated with NF1?
As NF1 develops, it can form benign (noncancerous) tumors called plexiform neurofibromas (PNs). In rare cases, however, it can also form tumors that are malignant (cancerous).
Why should caregivers look out for plexiform neurofibromas (PNs)?
Plexiform neurofibromas (PNs) are benign tumors that grow along a nerve. Between 30% and 50% of patients with NF1 develop plexiform neurofibromas (PNs).
In addition, studies show that patients with NF1 with plexiform neurofibromas (PNs) who are diagnosed and treated early may have better outcomes. Talk with your health care team if you notice any growths under your child’s skin.
Treatment for NF1 with Plexiform Neurofibromas (PNs)
Can surgery help treat plexiform neurofibromas (PNs)?
Sometimes, surgically cutting out a tumor may help reduce any symptoms that it is causing. However, due to their size and locations (near nerves and vital organs), many plexiform neurofibromas (PNs) are considered “inoperable,” meaning that they cannot be removed with surgery without devastating consequences to the life of the patient. A surgeon will help decide if removing a tumor is possible.
How is NF1 treated?
NF1 is usually treated by a team of doctors and health care specialists, including geneticists, neurologists, oncologists, surgeons, and other providers who specialize in treating symptoms related to NF1 and plexiform neurofibromas (PNs).
Currently, there are no FDA-approved medications for plexiform neurofibromas (PNs).
How are plexiform neurofibromas (PNs) typically treated?
In some cases, surgical reduction of tumors (also known as “debulking”) may be possible. In certain instances, debulking has been shown to reduce symptoms caused by plexiform neurofibromas (PNs).
Surgery to remove plexiform neurofibromas (PNs), however, may be linked to complications. The tumors are closely intertwined with nerves and can be located near major organs, which can cause complications. Also, many plexiform neurofibromas (PNs) tend to grow back after surgery.
Your doctor may prescribe therapy or medicines to help the symptoms of NF1 with plexiform neurofibromas (PNs), which can include:
- Pain
- Lack of mobility and diminished range of motion
- Depression
Living with NF1 with Plexiform Neurofibromas (PNs)
How does NF1 with plexiform neurofibromas (PNs) affect patients and caregivers?
NF1 with plexiform neurofibromas (PNs) can have a profound impact on childhood. Understanding the effects of the disease may help you prepare and equip your child with coping strategies.
NF1 with plexiform neurofibromas (PNs) can lead to physical and emotional issues:
- Restricted motion, which impacts physical mobility, range of motion, and strength
- Pain and visible physical changes, as plexiform neurofibromas (PNs) can grow in different sizes and in different parts of the body, including the face and neck
- Psychosocial problems, such as learning development and behavioral issues, can affect up to 50% of children with NF1
- Social isolation and psychological distress are common due to the visible nature of this disease
- Emotional stress can significantly affect patients, caregivers, and family members
Tips for helping your loved one with NF1 and plexiform neurofibromas (PNs):
- NF1 and its symptoms can cause a lot of uncertainty. Creating daily routines for children can help them feel secure and give them a positive sense of control
- Developing an honest and trusting relationship is important for all parents and children but is particularly important when coping with an NF1 diagnosis
- Building a supportive home environment, in which all family members are treated equally with respect and acceptance, can benefit not only the child with NF1, but also siblings who may feel that they get less attention from parents
- Helping children build their self-esteem is important because of the emotions associated with the visible physical changes of NF1, feelings of self-consciousness, and the social isolation that can happen as a result
- Making the transition from childhood to teenage years can be especially difficult when living with NF1. Helping children gradually take more control over their health care, medications, and treatment decisions can encourage responsibility and help them feel empowered
How can caregivers stay strong?
Frustration, worry, and anger are natural when someone we love is struggling with a difficult medical condition. It’s important that you:
- Learn all you can about NF1 with plexiform neurofibromas (PNs); knowledge is power
- Get professional help if you have significant changes in your mood and/or energy levels. You may have depression, which is common
- Explore healthy coping methods, such as meeting with supportive friends and learning to meditate
- Take time for yourself; joining a support group may help
- Let friends lend a hand; no one expects you do to everything by yourself


